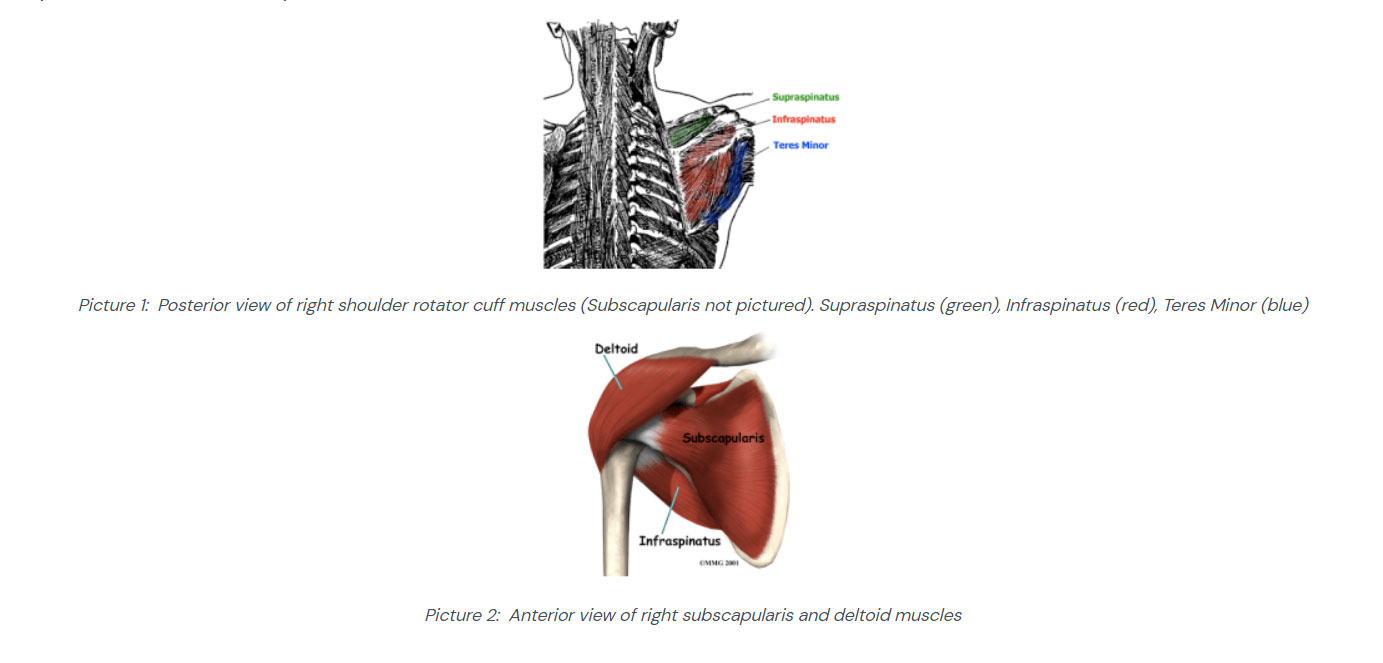
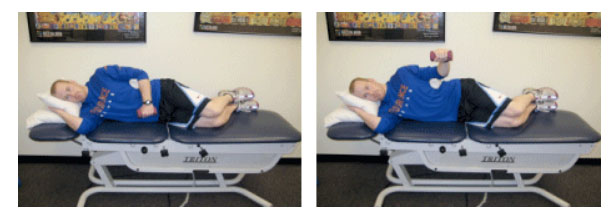
SHOULDER INJURY PREVENTION: PART 1
By Brandon Penas, PT
Repetitive overhead throwing places significant mechanical stress on both the shoulder and elbow joint, which can lead to anatomic changes in the underdeveloped athlete. Shoulder and elbow joint injuries occur primarily due to the body’s inability to control motion segments throughout the body during the throwing/pitching delivery. Such lack of control, coupled with overuse, can lead to further structural damage in the throwing upper extremity. Therefore, coaches and parents must be able to recognize and prevent overuse in young children in order to avoid injury. Past and current research in overhead throwing injuries has focused primarily on the factors contributing to injury. Both intrinsic (age, race, gender) and extrinsic (pitch count, pitch type, showcase participation) factors have been included in such research. Although intrinsic factors are important, they are not modifiable; therefore, the modifiable, extrinsic factors will be discussed in further detail as they relate to injury.
Pitch Count
In 2001, Lyman et al. published a longitudinal study of shoulder and elbow pain in youth baseball pitchers between the ages 9-12. One area of interest related to the number of pitches thrown in games and throughout a season by youth pitchers. The results of the study showed a direct association: as the number of pitches during a game increased, the occurrence of shoulder pain increased. Moreover, a direct association was also discovered between the number of pitches thrown during the season and elbow pain among the same age group: as pitch count increased throughout the season, the occurrence of elbow pain increased4,5. Such research reiterates the importance of tracking the number of pitches thrown by young pitchers during games and the entire season. Pitch counts should pertain to “in competition” or “game intensity” pitches, and should strive to create single game, weekly, and annual pitch count limits for young pitchers. Table 1 presents a general guideline to follow as it relates to the player’s age and number of pitches per game:
Table 1: Age-Related Pitch Counts:
| 8 to 10 |
50 |
| 11 to 12 |
60 |
| 13 to 14 |
75 |
| 15 to 17 |
90 |
The number of pitches thrown will be different between starting pitchers and relievers. Relievers who throw multiple days per week should be kept on a weekly pitch count, and should avoid throwing more than two days in a row without a day of rest. Starting pitchers, on the other hand, should be kept on a “pitches per game” pitch count, and be allowed at least 3-4 days of rest in between games pitched. A gradual increase in pitch count limit should be allowed as the age and level of play of the athlete progresses. Remember, it’s the number of pitches that’s important, not the number of innings pitched!
Pitch Type
Every young pitcher wants to have a curveball like Barry Zito, a split finger fastball like Roger Clemens, or a slider like Randy Johnson. Having an off speed pitch in your “repertoire” as a young pitcher makes it easier to get underdeveloped hitters out. However, over time, early exposure to such pitches places an even greater demand on the immature throwing arm and can lead to joint pain and injury. Research indicates the curveball is the most dangerous and difficult pitch to learn, as it requires large forces and torques at the shoulder and elbow with significantly different mechanics than the fastball1,2. Early emphasis should be placed on proper mechanics of the fastball and change-up and progressed to include the importance of location and change of speed. Table 2 presents a general guideline to follow as it relates to the type of pitch thrown and at what age it should be incorporated:
Table 2: Age-Related Pitch Types
| Fastball |
8 |
| Change Up |
10 |
| Curveball |
14 |
| Slider |
16 |
| Split Finger |
17 |
It’s important to remember that as the pitcher’s age and level of skill increase so do the forces at the elbow and shoulder joint with the pitching motion. Therefore, pitching mechanics and skill training are vital in overhead injury prevention, which will be discussed in greater detail in subsequent articles.
Strength and Conditioning
Although strength and flexibility of the throwing shoulder and elbow are important, core and leg strength and endurance also play an important role in determining a pitcher’s susceptibility to injury. Research has estimated that over 55% of the kinetic energy and momentum needed to throw a baseball comes from the legs and lower trunk6. The kinetic energy, or energy due to motion, begins in the lower extremities and is transferred through the trunk and throwing shoulder/arm throughout the pitching motion. Thus, if the pitcher’s legs and trunk begin to fatigue he/she produces less kinetic energy in the lower extremities and will rely on the shoulder to “make up” for the difference, which places added stress on the throwing shoulder/elbow. In an underdeveloped, underprepared, and overused pitcher, this state of fatigue can have unforgiving consequences. Most of today’s youth baseball players play multiple positions throughout the season. While some players excel as pitchers, they can’t pitch every game and, more importantly, need a break from pitching during the season! That being said, strength and conditioning programs for youth baseball players should aim to train the player both as a pitcher and position player simultaneously. Young baseball athletes should incorporate a well-balanced combination of strength, flexibility, endurance, and body awareness exercises/drills. Moreover, it’s important to expose these athletes to a stepwise progression related to age and avoid excessive training in only one area. Table 3 presents a general guideline to follow as it relates to the player’s age and strength training guidelines:
Table 3: Age-Related Strength Training Guidelines3
| 7 or younger |
No weight resistance, body weight exercises only. Emphasize technique. Introduce Stretching. Make it FUN! |
| 8 to 10 |
Core exercises emphasizing balance, proprioception. LIGHT resistance exercises. Scapular program. Keep it SIMPLE! |
| 11 to 13 |
Progressive resistance exercises: bench, pulldowns, rows. Begin focus on rotator cuff and scapula. Core and lower extremity strengthening. Control volume to avoid overuse! |
| 14 to 15 |
Total body focus with sport-specific training. Introduce plyometrics. |
| 16 or older |
Advanced strengthening and flexibility. Thrower’s 10 program and plyometrics. |
Seasonal Participation
Pitching outside of the player’s primary league (i.e. showcases, traveling teams, All-star tours) increases the number of pitches throw, thus increasing the risk of overuse injury. Coaches and parents should attempt to limit pitching to 9 months per year with at least 3 months off from pitching in order to decrease the risk of arm injury. At a young age it’s important to limit the pitcher to one team per season!
References
1. Elliott B, Grove JR, Gibson B, Thurston B: Three-dimensional cinematographic analysis of the fastball and curveball pitches in baseball. Int L Sport Biomech 1986; 2:20-28.
2. 2. Escamilla RF, Fleisig GS, Barrentine SW, Zheng N, Andrews JR: Kinematic comparisons of throwing different types of baseball pitches. J Appl Biomech 1998; 14:1-23.
3. Palleta, George. Injury Prevention and Treatment Techniques. Major League Baseball Medicine Conference. St. Louis, MO. January 3-5, 2008.
4. Lyman S, Fleisig GS, Waterbor JW, Funkhouser EM, Pulley L, Andrews JR, Osinski ED, Roseman JM. Longitudinal study of elbow and shoulder pain in youth baseball pitchers. Med Sci Sports Exerc., Vol 33, No 11 2001, pp. 1803-1810.
5. Lyman S, Fleisig GS, Andrews JR, Osinski ED: Effect of pitch type, pitch count, and pitching mechanics on risk of elbow and shoulder pain in youth baseball pitchers. AM J Sports Med 2002; 30:463-468.
6. Wilk, Kevin E: Restoration of Functional Motor Patterns and Functional Testing in the Throwing Athlete. Proprioception and Neuromuscular Control in Joint Stability. 2000:415-419.